CMS-0057-F Interoperability Suite for Payers
Move beyond compliance to scalable, real world interoperability—powered by the Availity Network.
Move beyond compliance to scalable, real world interoperability—powered by the Availity Network.

The Centers for Medicare & Medicaid Services Interoperability & Prior Authorization Final Rule (CMS-0057-F) establishes a baseline for interoperability by requiring payers to make data available through Fast Healthcare Interoperability Resources (FHIR®) APIs. But standing up APIs alone doesn’t deliver meaningful value.
Point-to-point integrations are costly to build, difficult to maintain, and nearly impossible to scale. Teams spend more time managing connections than improving clinical and operational performance.
Availity delivers everything CMS-0057-F requires—and the network connectivity to make it work in practice. Our end-to-end interoperability suite combines compliant FHIR APIs, workflow automation, and data orchestration on a trusted national network, enabling payers to scale interoperability, accelerate adoption, and realize measurable value beyond compliance.
An End-to-End CMS-0057-F Solution—Built on a Live Network
Availity connects your APIs, workflows, and partners through a single interoperability framework—reducing fragmentation while accelerating adoption across providers and payers.
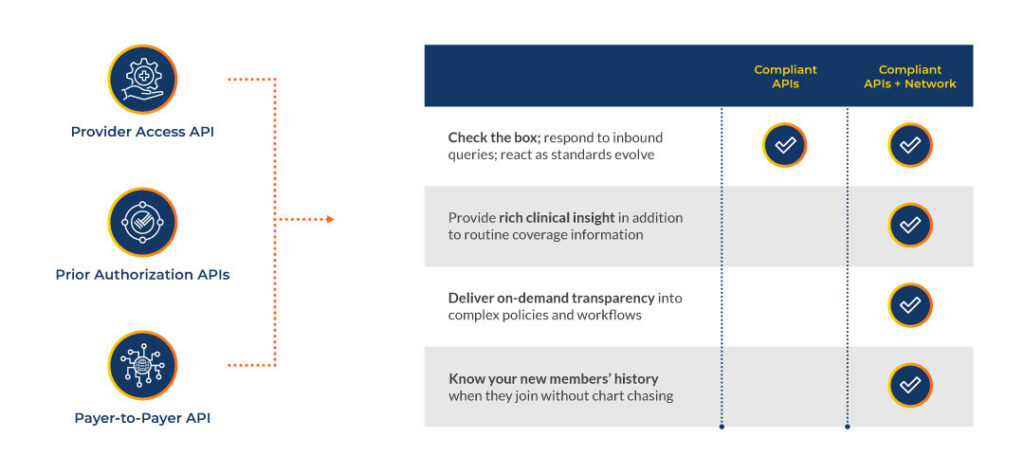
APIs Enable Compliance. Networks Unlock Value.

Building compliant FHIR APIs checks the regulatory box—but compliance alone delivers limited return. Interoperability creates value only when APIs are activated through network connectivity.
When data moves reliably across organizations; workflows evolve, and insights become actionable at scale.
Use Cases Powered by Availity Clinical Data Solutions

CMS-0057-F compliant connectivity between providers, partners, and your CRD/DTR/PAS APIs.
Provides a secure, standardized onramp between providers, partners, and your CRD/DTR/PAS APIs—enabling CMS-0057-Fcompliant prior authorization at scale.
Orchestrate, normalize, and scale utilization management workflows.
Absorbs orchestration, normalization, and enrichment complexity—allowing payers to modernize utilization management while reducing operational burden.
Secure, standardized provider access to patient data under CMS-0057-F.
Enables secure, CMS-0057-F compliant provider access to patientspecific data through a single, standardized entry point.
One-to-many payer data exchange at real world scale.
Provides a standardized gateway for exchanging clinical, claims, and authorization data between health plans—supporting CMS-0057-F at real-world scale.
Connected
Providers
Direct Payer
Connectivity
Connect
B2B Partners
Billed Claims
Annually
US Healthcare
Transactions
CMS‑0057‑F is the CMS Interoperability and Prior Authorization Final Rule that requires payers to support standardized FHIR APIs for prior authorization, provider access, patient access, and payer‑to‑payer data exchange.
Availity delivers a compliance‑ready CMS-0057-F solution anchored in network connectivity, combining FHIR‑based APIs with connectivity hubs that enable data exchange at scale across payers and providers.
Yes. Many payers choose to build or partner (including with Availity) on their own APIs. Availity complements those APIs by providing the connectivity, routing, onboarding, monitoring, and operational support required to make them work in the real world.
APIs alone don’t ensure adoption. CMS-0057-F success depends on many‑to‑many connectivity, provider onboarding, standardized routing, performance monitoring, and ongoing support—capabilities delivered through Availity’s national network.
Availity supports CMS-0057-F prior authorization through Da Vinci–aligned CRD, DTR, and PAS workflows, paired with network connectivity that standardizes how requests flow across providers, EHRs, and payer systems.
Availity enables CMS-0057-F compliant Provider Access by providing a Provider Connectivity Hub that supports authentication, routing, monitoring, and high‑volume provider access to patient‑specific data.
Availity provides a one‑to‑many Payer‑to‑Payer Connectivity Hub, reducing point‑to‑point integrations and enabling secure, scalable data exchange between health plans under CMS-0057-F requirements.
CMS-0057-F can feel overwhelming without a clear path. Availity helps payers move from uncertainty to execution by combining regulatory guidance, proven connectivity models, and a practical roadmap for standing up compliant, scalable interoperability.
Check out our CMS-0057-F Blueprint for more information here
Fill out the form below and we will get back with you.