The State of Payer-Provider Collaboration
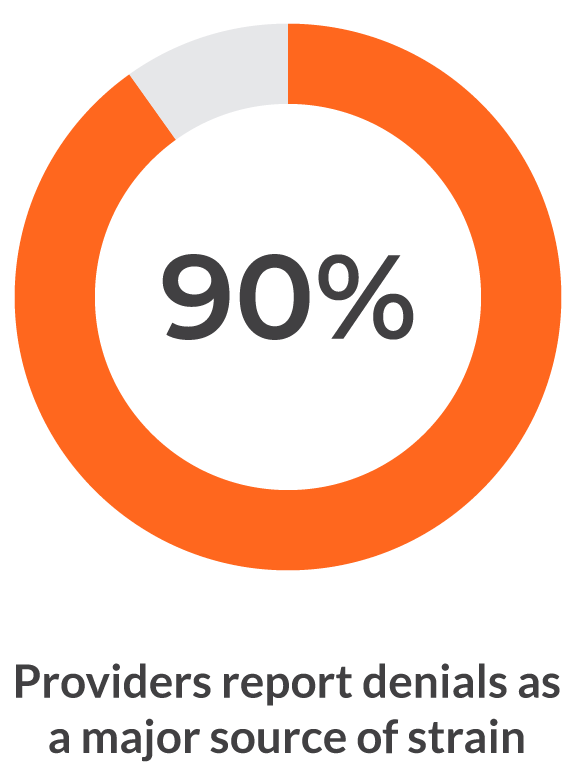
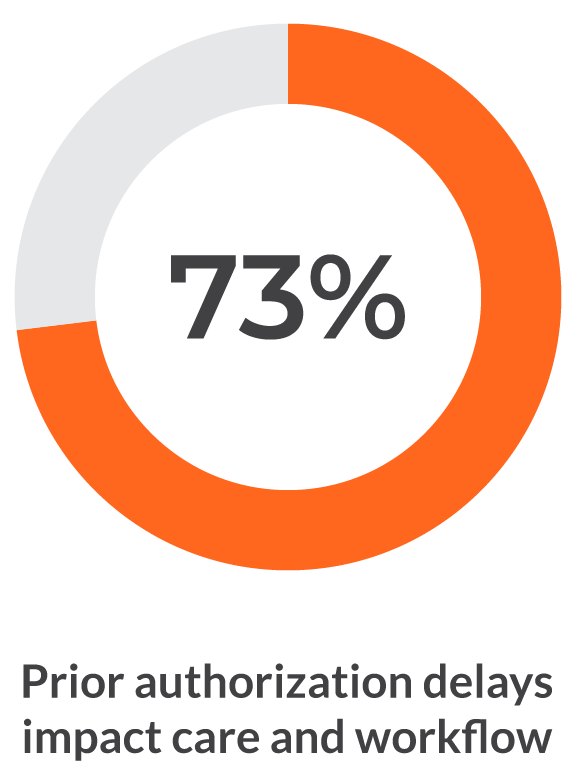
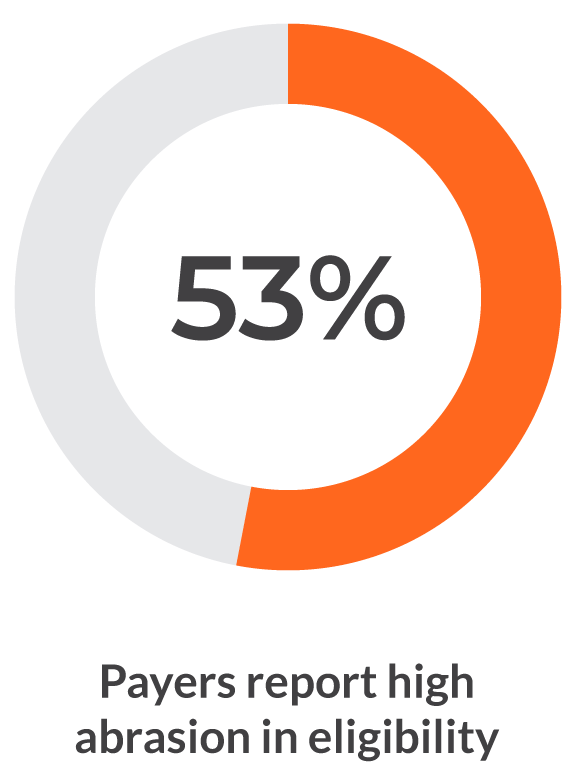
The Availity Abrasion Index 2026 quantifies where workflows breakdown across eligibility, prior authorization, claims, and denials, and what those failures are costing health plans and providers.
Based on research across payer and provider organizations

What you’ll find in the report
A clear, data-backed view of where payer-provider workflows breakdown and how those issues create downstream cost, delay, and rework.
Where abrasion is highest
across key workflows
Where payers and providers
align—and where they don’t
How breakdowns create
downstream impact
Practical insights to reduce
administrative burden
Breakdowns across healthcare workflows
Built from payer and provider perspectives, the Abrasion Index shows where workflows align, where they breakdown, and what drives those issues.
Reduce administrative burden across payer-provider workflows
See where workflows breakdown across eligibility, prior authorization, claims, and denials and how those issues create downstream cost, delay, and rework.