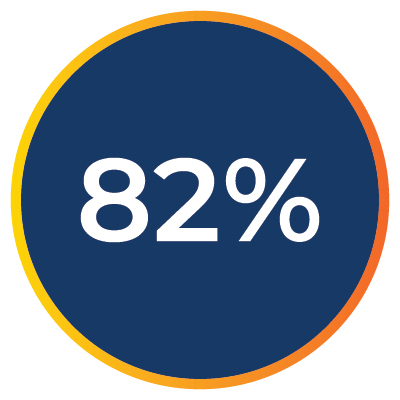
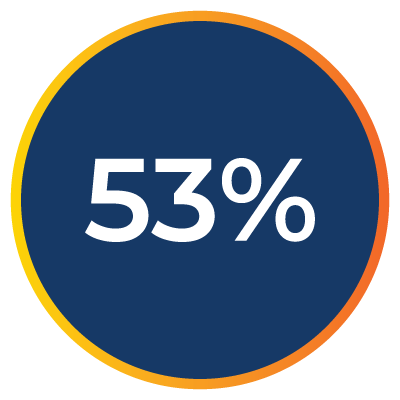
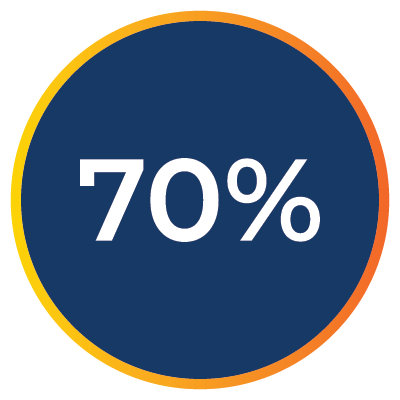
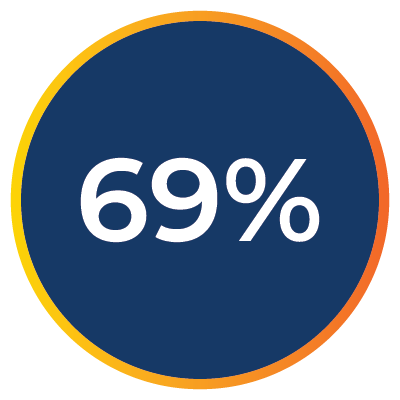
of providers agree initial denials and payer response times lead to delays in care.
- Portal Login
-
-
SolutionsBack
Solutions
-
For Payers
Simplify complex processes and improve payer-provider collaboration.
BackFor Payers
-
The Availity Platform for Payers
Simplify complex processes and improve payer-provider collaboration.
-
Network Connectivity for Payers
Connect to the most providers and HIT partners nationwide.
-
Multi-Payer Portal
Improve collaboration with your provider network by automating core workflows.
-
Intelligent Utilization Management
Help ensure the right care at the right time by transforming the prior authorization process.
-
Payment Accuracy
Reduce administrative waste by shifting edits early in the claim lifecycle.
-
Clinical Data Solutions
Make clinical data work for you by streamlining acquisition, improving quality, and optimizing workflows.
-
Provider Lifecycle Solutions
Improve the quality of provider data for use across the enterprise.
-
Digital Correspondence
Drive cost out of provider communications by digitizing paper correspondence.
-
CMS-0057-F Solution Suite
Operationalize 0057 with compliant FHIR APIs and scalable interoperability on a trusted national network.
-
The Availity Platform for Payers
-
For Providers
Streamline workflows, reduce denials, and ensure accurate payments.
BackFor Providers
-
The Availity Platform for Providers
Streamline workflows, reduce denials, and ensure accurate payments.
-
Network Connectivity for Providers
Improve revenue cycle performance with fast and secure connections to payers nationwide.
- Revenue Cycle Management
-
The Availity Platform for Providers
-
For HITs
Seamlessly deliver complete and accurate healthcare information.
BackFor HITs
-
Health IT Overview
Solutions for healthcare technology companies—from foundational connectivity to network‑powered innovation.
-
Clearinghouse & Trading Partner Network
National‑scale transaction processing and trusted connectivity across eligibility, claims, and payments.
-
Availity Extend
Modern developer experience and agent‑ready orchestration layer for building and automating real healthcare workflows on the Availity network.
-
Health IT Overview
-
For Payers
-
ResourcesBack
Resources
-
Insights
Back
Insights
-
Blog
Get the latest industry insights.
- Insourcing Utilization Management
-
Customer Success Stories
See success stories from our customers.
- Insourcing Blueprint
- Availity Rapid Recovery
- CMS-0057-F Readiness Blueprint
- Infographics
- Abrasion Index
-
Blog
- Partner Resources
- Payer Lists
-
Insights
-
About
-
ConnectBack
Connect
-
Locations
See where we're located.
-
Contact Sales
Find the best way to get in touch.
-
Customer Support
Get in touch with customer support.
-
Events
Learn about upcoming industry events.
-
Locations
-